Clinical Assessment for Addiction is a systematic process that evaluates an individual’s substance use alongside physical, mental, and psychosocial factors to determine the severity of addiction and guide personalized treatment plans.
According to the chapter on Clinical Assessment, In Management of the Addicted Patient in Primary Care (pp. 28-54). (2007), substance use disorder (SUD) detection remains a significant challenge in primary care settings, with 90% of primary care physicians failing to identify addiction even when patients present classic symptoms. This finding highlights a critical gap in diagnosis, particularly given that patients may exhibit both obvious and subtle indicators of addiction during routine visits.
Clinical assessments and diagnosis help identify mental health conditions and set appropriate care levels, ensuring personalized and effective treatment.
The clinical assessment process involves quick intake, screening, and evaluations of substance use, overall health, and social background for a complete treatment plan.
Assessment tools and techniques rely on interviews, questionnaires, structured DSM 5 assessments, and biological tests to build a comprehensive profile. Dual Diagnosis Assessment detects both addiction and co-occurring mental health issues, enabling integrated treatment that minimizes relapse risk.
What is an Addiction Assessment?
Addiction assessment is the process of systematically evaluating an individual’s substance use and related behaviors to determine the presence, severity, and impact of addiction. It involves gathering information about the individual’s substance use history, patterns, and associated factors, as well as assessing their physical health, mental health, and psychosocial context.
Addiction assessment provides a comprehensive understanding of the individual’s addiction and its underlying factors, which guides treatment planning and intervention strategies. It involves clinical interviews, self-report questionnaires, screening tools like the DSM-5, physical examinations, psychological assessments, and collaboration with the individual to gather accurate and relevant information.
ASAM provides criteria as well as the DSM-5 Diagnostics and Statistical Manual which guide clinicians, doctors, and nurses to assess patients for their appropriateness in treatment.
What is the Importance of Clinical Assessments and Diagnosis in Addiction Rehab?

The importance of clinical assessments and diagnosis in addiction rehab includes creating personalized treatment strategies, identifying concurrent mental health conditions, establishing appropriate care levels, and monitoring recovery progress. From determining underlying trauma factors to implementing evidence-based interventions, these evaluations form the foundation for effective treatment outcomes.
Here are the key roles of clinical assessments and diagnosis in addiction rehab:
Tailoring Treatment
Clinical assessments help treatment providers understand the unique needs, challenges, and underlying factors contributing to an individual’s addiction. This information allows them to develop personalized treatment plans that address specific issues and promote effective recovery.
Identifying Co-occurring Disorders
Many individuals with addiction also experience co-occurring mental health disorders. Clinical assessments help identify these dual diagnoses, allowing for integrated treatment approaches that address both addiction and mental health simultaneously. This comprehensive approach improves treatment outcomes and reduces the risk of relapse.
According to SAMHSA’s 2022 report, In the USA, approximately 21.5 million adults have a co-occurring disorder.
Determining Treatment Levels and Interventions
Through assessments, treatment providers determine the appropriate level of care and interventions needed for each individual. This ensures that individuals receive the right intensity of treatment, whether it be outpatient, inpatient, or a combination, based on the severity of their addiction and other clinical factors.
Monitoring Progress and Adjusting Treatment
Clinical assessments provide a baseline for measuring progress throughout the treatment journey. By regularly reassessing individuals, treatment providers track their advancements, identify any barriers or challenges, and make necessary adjustments to the treatment plan to optimize outcomes.
Addressing Underlying Factors
Addiction is connected to underlying issues such as trauma, past experiences, or social factors. Clinical assessments help uncover these underlying factors, enabling treatment providers to address them directly, leading to more comprehensive and lasting recovery.
Enhancing Treatment Effectiveness
By gathering detailed information about an individual’s substance use history, physical health, mental health, and psychosocial background, clinical assessments enable treatment providers to develop interventions that are specific, evidence-based, and tailored to address the individual’s unique needs. This personalized approach enhances treatment effectiveness and increases the chances of successful recovery.
What is the Clinical Assessment Process for Addiction Rehab?

The clinical assessment process for addiction includes comprehensive intake screening, detailed substance use history evaluation, mental health disorder identification, physical health examination, and psychosocial background analysis. Our experienced treatment professionals utilize validated assessment tools and collaborative approaches throughout this process to develop personalized recovery plans.
The clinical assessment process includes the following key steps:
Intake and Screening
The process begins with gathering basic information about the individual, including personal details, contact information, and reasons for seeking treatment. Screening tools assess the severity of substance use and determine the appropriate level of care.
Substance Use History
A thorough exploration of the individual’s substance use history occurs. This includes detailed questions about substance types, frequency, duration, patterns of use, and previous treatment experiences. Understanding the individual’s relationship with substances provides valuable insights into addiction’s nature and severity.
Co-occurring Mental Health Assessment
Mental health significantly impacts addiction. A comprehensive assessment identifies co-occurring mental health disorders through standardized questionnaires, clinical interviews, and assessment tools to detect symptoms of anxiety, depression, trauma, or other conditions.
Physical Health Evaluation
The assessment of the individual’s physical health identifies substance-related medical complications or underlying health issues. This evaluation includes a physical examination, laboratory tests, or consultations with medical professionals to address immediate health concerns and inform the treatment plan.
Psychosocial Assessment
A psychosocial assessment explores various aspects of the individual’s life, including social support systems, family relationships, employment or educational history, housing situation, legal issues, and psychosocial stressors. This assessment identifies contextual factors contributing to addiction or impacting the recovery process.
Validated Assessment Tools
Throughout the assessment, validated assessment tools and questionnaires gather standardized information and measure specific aspects of addiction and mental health. These tools provide objective data and guide treatment decisions.
Collaboration and Information Sharing
The assessment process involves collaboration between the individual and assessing professionals. Building rapport, establishing trust, and creating a safe, non-judgmental environment fosters open communication. The individual’s input and self-reporting are crucial for accurate information gathering.
Documentation and Diagnosis
Treatment professionals document assessment findings and make diagnoses based on established criteria from the Diagnostic and Statistical Manual of Mental Disorders (DSM-5). Diagnosing co-occurring disorders is essential for developing an integrated treatment plan.
Treatment Planning
Assessment findings serve as the foundation for developing an individualized treatment plan. Treatment providers collaborate with the individual to set treatment goals, determine appropriate interventions, and identify specific needs or preferences.
The clinical assessment process is an ongoing and dynamic part of addiction rehab. It helps treatment providers gain a holistic understanding of the individual’s addiction, mental health, physical health, and psychosocial context.
What Tools and Techniques are Used in Assessment for Addiction Rehab?

Tools and techniques used in assessment for addiction rehab include comprehensive clinical evaluations, standardized screening instruments, diagnostic interviews, and biological testing methods. These encompass face-to-face consultations, validated questionnaires, structured assessments, and laboratory analyses to determine substance use patterns and severity.
Here are the most common tools and techniques used in assessment for addiction rehab:
- Clinical Interviews: Face-to-face interviews between the individual and a trained clinician or addiction specialist are conducted to collect detailed information about the individual’s substance use history, patterns, and associated factors.
- Self-Report Questionnaires: Standardized questionnaires are administered to individuals to assess the severity of substance use, measure addiction-related behaviors and symptoms, and evaluate mental health symptoms. Examples include the Addiction Severity Index (ASI), the Substance Abuse Subtle Screening Inventory (SASSI), and the Beck Depression Inventory (BDI).
According to Samet, S.’s 2007 study, ‘Assessing addiction: concepts and instruments.’, the time required for addiction diagnosis varies significantly based on the chosen evaluation instrument. The Addiction Severity Index (ASI) is relatively brief at 45-60 minutes plus 10-20 minutes for scoring, while the Composite International Diagnostic Interview (CIDI) takes 75 minutes. More comprehensive tools like the Structured Clinical Interview for DSM-IV (SCID) require 90 minutes, and the most detailed instrument, the Psychiatric Research Interview for Substance and Mental Disorders (PRISM), needs 120 minutes for complete administration. These standardized timeframes help rehabilitation centers plan their intake processes effectively. - Substance Use Screening Tools: Screening tools, such as the Alcohol Use Disorders Identification Test (AUDIT) and the Drug Abuse Screening Test (DAST), are used to assess the extent and impact of substance use.
- Structured Clinical Assessments: Structured clinical assessments, such as the Diagnostic Interview for DSM-5 (SCID), are used by trained clinicians to assess for substance use disorders and co-occurring mental health conditions.
- Urine or Blood Tests: Toxicology screenings, such as urine or blood tests, are used to detect the presence of drugs or alcohol in an individual’s system.
What is the DSM 5 Diagnosis for Addiction (Diagnostic Criteria for Addiction)?
The DSM-5 diagnosis for addiction includes specific diagnostic criteria that help clinicians identify and assess substance use disorders. These diagnostic criteria, established by the American Psychiatric Association in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), provide the standard framework for diagnosing addiction in clinical settings.
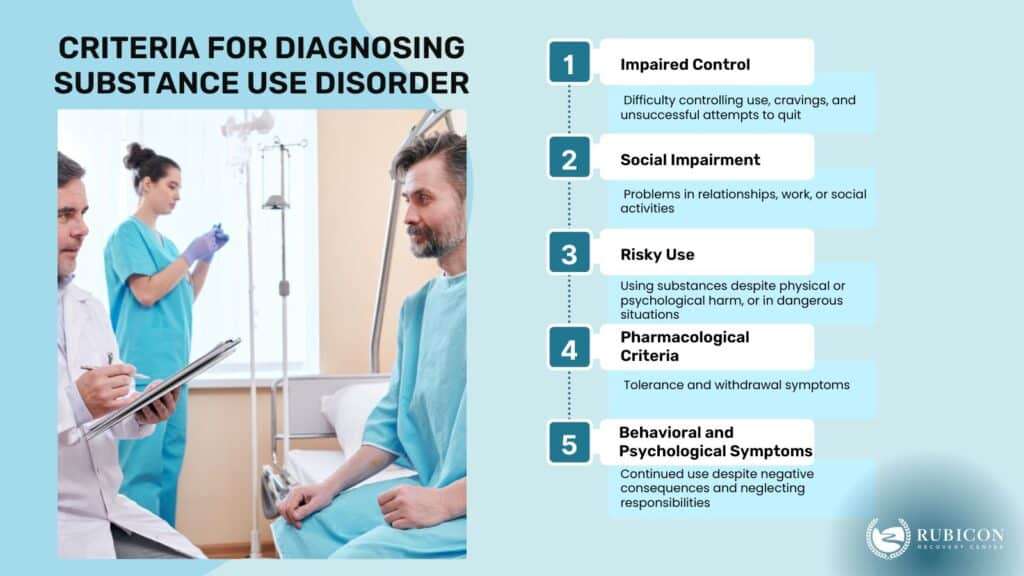
The criteria for diagnosing SUD include the following:
1. Impaired Control
The individual experiences difficulty controlling their substance use, such as using larger amounts or for a longer duration than intended, unsuccessful attempts to cut down or quit, spending a significant amount of time obtaining or recovering from substance use, and experiencing intense cravings.
2. Social Impairment
Substance use leads to recurrent problems in the individual’s social, occupational, or educational functioning. This includes strained relationships, poor performance at work or school, or withdrawal from previously enjoyed activities and social engagements.
3. Risky Use
The individual continues to use substances despite being aware of the resulting physical or psychological problems. Risky use involves using substances in physically hazardous situations, such as while driving or using substances despite having a co-occurring physical or mental health condition that is exacerbated by substance use.
4. Pharmacological Criteria
The individual develops tolerance and withdrawal symptoms associated with substance use. Tolerance refers to needing larger amounts of the substance to achieve the desired effect, while withdrawal refers to experiencing physical or psychological symptoms when substance use is discontinued or reduced.
5. Behavioral and Psychological Symptoms
The individual experiences a range of behavioral and psychological symptoms that indicate the presence of addiction. Behavioral and psychological symptoms include diminished interest in other activities, continued substance use despite negative consequences, preoccupation with obtaining and using substances, and neglecting important obligations and responsibilities.
The DSM-5 provides a severity rating for SUD based on the number of criteria met: mild (2-3 criteria), moderate (4-5 criteria), or severe (6 or more criteria). It is important to note that the DSM-5 recognizes that addiction exists on a spectrum and that the severity of SUD varies from person to person.
What is the Importance of Dual Diagnosis Assessment in Addiction Rehab?
The importance of dual diagnosis assessment in addiction rehab includes comprehensive evaluation of co-occurring mental health conditions, development of personalized treatment strategies, and implementation of targeted interventions for lasting recovery. Our experienced clinical team conducts thorough assessments to identify conditions like depression, anxiety, PTSD, or bipolar disorder that accompany substance use disorders. This integrated approach allows us to create more effective treatment plans that address both addiction and mental health simultaneously
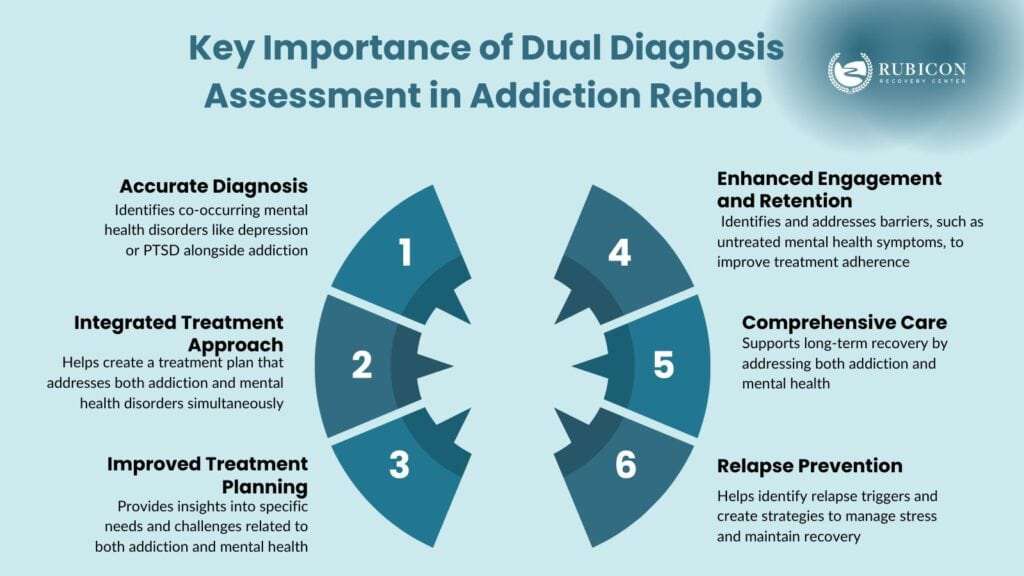
Here are the key importance of dual diagnosis assessment in addiction rehab:
- Accurate Diagnosis: Many individuals with addiction also experience co-occurring mental health disorders, such as depression, anxiety, bipolar disorder, or post-traumatic stress disorder (PTSD). Dual diagnosis assessment allows for the accurate identification and diagnosis of these co-occurring disorders.
- Integrated Treatment Approach: Dual diagnosis assessment helps inform the development of an integrated treatment approach that addresses both addiction and co-occurring mental health disorders concurrently.
- Improved Treatment Planning: Dual diagnosis assessment provides critical information for treatment planning. It helps treatment providers understand the specific needs, challenges, and underlying factors associated with both addiction and mental health disorders.
- Enhanced Treatment Engagement and Retention: Dual diagnosis assessment identifies barriers, such as the presence of untreated mental health symptoms, and allows treatment providers to address them proactively.
- Comprehensive Care: By addressing both addiction and mental health, treatment providers support individuals in achieving sustainable, long-term recovery.
- Relapse Prevention: Dual diagnosis assessment helps identify the factors that contribute to relapse and develop strategies to prevent it, helping individuals better manage triggers, cope with stress, and maintain their recovery in the face of challenges.
What Therapies Are Used In Rehab After The Assessment?
The therapies used in rehab after the assessment typically include Cognitive Behavioral Therapy (CBT), group and individual counseling, family therapy, motivational interviewing, and holistic approaches like meditation and yoga. These evidence-based therapies work together to address the underlying causes of addiction while helping patients develop essential coping strategies for long-term recovery.
How Is A Clinical Assessment Different From A Self-assessment?
The key difference between a clinical assessment and a self-assessment lies in their professional execution and comprehensiveness. Clinical assessments are conducted by qualified healthcare professionals who use standardized tools to evaluate substance use, mental health, and medical history. These assessments provide comprehensive, objective insights and are specifically designed to guide treatment planning. Self-assessments involve individuals evaluating their own substance use patterns. Self-assessments lack objectivity and overlook important aspects of addiction or co-occurring disorders. Self-assessments serve as an important first step toward recognizing substance use issues and seeking help. However, self-assessments do not replace the thorough evaluation provided by professional clinical assessment.
